The power of diet, hope and remission from diabetes type 2.
Below is a modified version of an article soon to be published in various association magazines on a recent study on the treatment of diabetes with a low carb diet in an NHS GP surgery:
https://nutrition.bmj.com/
The NHS currently spends £1.5 million an hour or 10% of its total budget on diabetes.
This totals an estimated 11.7 billion a year for treatment of diabetes type 2 itself and critically the complications of diabetes, with the latter representing a more significant amount. Over 8 billion of the total figure is for in-patient care arising from complications.
These figures do not take into consideration the cost of work absenteeism, early retirement or social benefits, which total 15.4 billion a year.
Every year these figures are going up and up and up.
However, NHS GP Dr David Unwin, founder of www.lowcarbprogram.com has been utilising a low carbohydrate diet (LCD) as treatment for diabetes in his clinic for many years and has recently published his results.
Over a period of eight years, the LCD was offered to all patients with an existing or new diagnosis of type 2 diabetes (T2D). Of those offered, 186 patients started a LCD, equalling 39% of his patients with T2D.
Patients were given educational materials plus, on average, three additional 10 minute appointments per year. They were also offered 90 minute evening group sessions every six weeks with relatives encouraged to attend.
Behavioural changes were employed, encouraging patients to consider their individual hopes and health goals, plus the hope of drug free remission for T2D.
The average age of patients was 63, with 33 months the average time on LCD.
They average weight loss of 10kg – let that one sink in !!
No counting calories, no bulls**t weekly weigh-ins with slimming world telling you about food “sins“, just eat real/whole food with an empasis on higher fat and protein and low(er) carbohydrate.
HbA1c (glycoslyated haemoglobin – a long term marker of blood sugar control, is effectively how sticky your haemoglobin is) dropped from 63 to 46 mmol/mol (note under 42 is normal, 42-48 pre-diabetic and over 48 diabetes).
Blood cholesterol levels fell on average by 0.5 mmol/L and triglycerides by 0.9 mmol/L – It is worth remembering that an LCD is also a high fat diet. It is often the overconsumption of highly processed carbohydrates which leads to an excess of sugar in the blood that must then be turned into fat that can lead to the elevation of cholesterol and triglycerides.
The overall remission rate was 51%, with that figure rising to 77% for those diagnosed within the last year.
Again, let that sink in – half of all T2D patients that agreed to change their diet in one NHS practice achieved remission.
Even those with a 15 year history had 20% remission rates.
Note even those still classified as diabetic had huge reductions in HbA1c.
The practice cost of diabetes per patient per year dropped to £4.94 while the national average is £11.30.
Think about that in terms of cost savings for the NHS spending 11.7 billion on diabetes a year.
How many billions could they reallocate to other services straining under the weight on the nation?
The discussion highlighted some interesting points to consider:
– Ongoing support was critical, the practice response to LCD has gone up and up since they gave more support in one to one sessions and in a group setting. This is both educational and accountability.
– Focusing on LCD as a lifestyle not a diet
-Discussions around food as an addiction helped patients with their relationship with food.
– Frank honesty about the importance of weight loss for health was key to the outcome.
In contrast to this, they note their less experienced colleagues worried that talking about obesity was “fat shaming” – this last point is absurd.
When did patient centred evidence-based medicine reduce itself to avoiding potential emotional upset about the reality of the patient’s health situation?
I suspect any feeling of emotional upset with the truth about obesity might be miniscule to the upset about having your legs amputated or going blind from uncontrolled diabetes.
Things they did not do which could increase results even further from the literature and my personal clinical experience.
Intermittent fasting – the 16-8 method is now well established as an effective way to help metabolic health. We have 24 hours in a day, fast for 16 and utilise a 8 hour feeding window.
For most people, the easiest way to employ this is by not eating breakfast, which is usually a very carbohydrate heavy meal. Break the fast around noon and consume 2 large, nutrient dense meals, with a focus on quality fat and protein, minimal carbohydrate with a low glycemic load.
Alternatively, two normal sized meals with snacks in between, aiming to to finish in the evening, usually around 8 pm.
This is relatively easy to do as it makes your morning routine easier, thus is very sustainable and helps avoid a traditionally high-carb meal.


We also know from multiple studies that eating your protein/vegetables in the meal first and carbohydrate/sugar last, we can drop blood glucose response in the hours after food by anything from 20-70%.
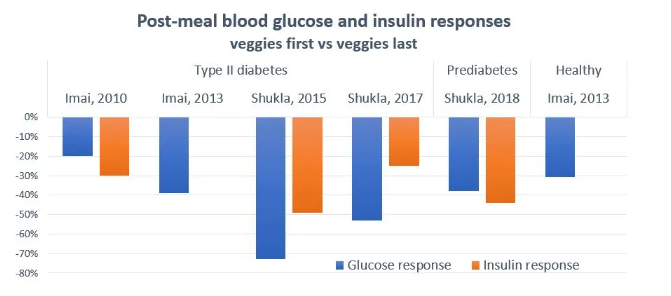
I can’t make it any easier than that, drop your blood sugar response by 70% just by eating your veggies first.
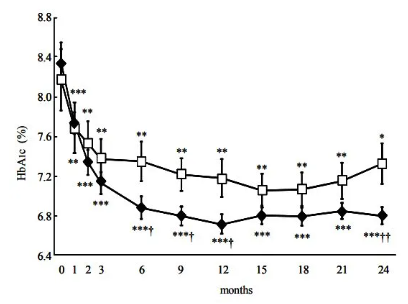
But even better than that we have real world data with the same interventions over 3-24 months, showing significant reductions in long term marker HbA1c, compared to diet alone, without ordered eating.
Open squares are diet change alone, food eaten as they wish. HbA1c plateaues at 3 months, while dark filled diamond are veggies first plus diet continues to drop for another 9 months.
Apple cider vinegar (with the mother) is a traditional food with many suggested benefits.
The acetic acid is an excellent addition to help blunt blood sugar spikes according to recent meta-analysis.


The acid also helps people digest better as many older patients are under producing stomach acid, which is critical for absorption of protein, minerals and B12.
The acidity from the stomach is also the trigger for release of bile and pancreatic enzymes, which are critical for fat absorption and proper breakdown of carbohydrate respectively.
And, of course, we would encourage exercise, a blend of traditional cardiovascular low level but also some high intensity internal training (HIIT).
The latter is often best performed on a stationary exercise bike depending on the neuro-mechancial health of the patient and allows really vigorous exercise to push the heart rate up for short periods.
HIIT has been shown to often work better for weight loss than traditional cardiovascular exercise.


Supplementally, chromium & alpha lipoic acid are both well evidence based interventions to help lower blood glucose levels and help restore insulin sensitivity.


Case study – Jenny is in her late 70’s, diagnosed as T2D in her early 50’s, and has a long history of yo-yo dieting using a low fat approach via weight watchers/slimming world. She uses metformin and three blood pressure medications, and is approximately 5 stones overweight.
She has tried a LCD before but failed as she struggled to increase her fat intake and ended up in a calorie deficit which led to binge eating. She refused to entertain the idea of not eating breakfast as she was always ravenously hungry upon waking and had been told it was the most important meal of the day.
She subscribed to the online LCD group www.lowcarbprogram.com and found the educational information, daily group webinars and forum invaluable.
By stabilising her daily blood sugar spikes with the high fat, LCD, she was also able to begin extending her fasting in the mornings from 12 hours out to 16.
This plus a regular exercise regime, eating her vegetables/protein first, carbohydrate last, & apple cider vinegar, over a period of 18-24 months, she lost 4.5 stones in weight.
With her GP’s consent, she was able to slowly reduce her metformin, and finally remove it all together. She also was able to stop two of her blood pressure medications and reduce by 50% the remaining medication. She was officially in remission from T2D when she turned 80.
I regularly refer patients to www.lowcarbprogram.com to get education and support in their quest for remission and health. At £14 a month, or £3.50 a week it represents excellent value and may be available as a “prescription” via their GP.
All too often, patients are simply given a prescription for metformin with no discussion on why they might be diabetic and how they might take an active role in their own health.
The very definition of encouraging dependence.
Given Dr Unwin’s remarkable success with a patient centred approach, we can only hope the NHS takes note, and the NICE guidance is modified to recognise remission is possible via diet (the root cause).
This could lead to huge saving of money, quality of life and additional years of life.

